The drastic start to feeding a child with CP
Feeding is a nightmare that never seems to end when your child has CP. There are so many obstacles. Where do I begin?
A few hours after the birth of Emma, I woke up in ICU. I was shocked to find an oxygen tube connected to my nose.
“I don’t need this, ” I thought as I tried to pull it off, but alarm bells started bleeping like mad. I quickly put them back and pretended to be asleep when the nurse came running. My mind was racing, I remembered my baby, but where was she? The doctor and nurses were so rushed during the birth that I never even saw her.
So I “woke up” and begged the ICU nurse to help me see my baby. After a few hours they brought me two things: a photograph of Emma in an incubator (I was too weak to visit her) and a breast pump. The photo was pinned to the drip stand and I was instructed to start pumping immediately. This is not a breastfeeding/pumping blog, but I will say that it was hard, very hard. Yet, to this day, I will never regret the pain that I went through during those months because it meant my daughter received breast milk. This is something I am particularly grateful for now that I know far more about the science of nutrition. But with this new knowledge, I’ve also developed many regrets.
The more I learn about nutrition in Cerebral Palsy, the more I realise how much more I could have done in those early days to optimise the therapy of Emma’s Cerebral Palsy in order to gain the most ground. There was even the thought that I could have prevented it if I was healthier during my pregnancy (this is a post for another day).
In the early days, once she was weaned off breast milk and I started solid food feeding, my focus was to give her nutrient-dense food. I gave her chocolate because chocolate contains fat, I gave her a lot of dairy, fatty cuts of meat and I turned a blind eye to sugar consumption. I tried to include fibre in her diet through whole grains (such as cereal and bread) but her fresh food intake was limited. She was sensitive to textures and couldn’t chew hard fresh fruit and vegetables. She simply refused most fresh food. A friend told me that his son, whose son has a similar level of CP to Emma’s, only eats sweet semolina porridge and nothing else – it’s really shocking but we all have major feeding obstacles with children like ours.
Grasping the magnitude of the problem
My doctor led me to believe that the problem was that she could not eat, chew or swallow food or fluid properly – so the skinny body is the result of a child not eating well. I have since – through a lot of reading – realised that there is a more balanced view to this. While the child does struggle with the mechanics of eating, the larger (more difficult to fix) challenge has to do with metabolic dysregulation. This is when the body doesn’t “understand” what to do with the food/nutrients it receives. The cause of this is complicated and I will have to address my understanding of it in a separate post. Here I will say that I don’t think this challenge is discussed enough with parents, and this is probably because, apart from diet and supplements, we don’t really know how to fix a system that is as dysregulated as the one we see in CP.
This is why so many of the articles that you may read say that because the feeding challenges are so extreme, every bite the child eats needs to “pack a punch”, i.e. feeding them a calorie-dense diet. But this isn’t a solution, and the major flaw is illustrated clearly when under-nourished children are given a feeding tube. They gain weight, yes, but they gain the wrong kind of tissue (fat tissue) instead of the desired healthy muscle. In addition, many CP kids struggle with brittle bones that can lead to fractures – and while many say this is due to lack of weight bearing, there is evidence that also says it’s in part due to nutritional shortages and poor metabolism. I am not suggesting tube feeding is a bad thing, for many kids it’s life-saving. What I am saying is that one will not achieve as much as one hopes for with a feeding tube when the metabolic dysregulation is not addressed as well.
The breakthrough
I started to realise the importance of nutrition and tissue quality (and what to do about it) when we started with ABR. One of the first tests the ABR practitioner did was to grab hold of the skin on Emma’s stomach to examine how much tissue there was – they looked at quality and quantity. They also tested the compressional strength of the tissues (see the photographs below for an illustration) I had never seen another doctor do this. They showed me how they were only able to grab loose skin and that the skin had no connection to the muscle underneath. This was astounding: my daughter had no adequate sub-cutaneous tissue, the type of tissue that connects your outer skin to the muscles and bones. And the problem didn’t end there – the deeper layers of tissue had a similar issue, they were not connecting to the bones they surrounded. Emma’s skin was sliding around over her body structures – she was truly just skin and bone, despite me spending hours a day feeding her. The ABR team woke me up to metabolic dysregulation in a big way. They claimed that their method of mechanical stimulation was able to address this metabolic problem and help bring regulation back to Emma’s system. The really great news is – they were right.
Fine-tuning the development
This wake-up call not only put me on the path to understanding more about nutrition and its effect on the body, but as we were seeing wonderful results with ABR in Emma, I wanted to see if I could optimise Emma’s ABR progress through diet. I read widely, from studies that saw how mechanical stimulation and nutritional supplements restored muscle function to lame rats to academic papers that looked at the muscle and connective tissue problems that were faced by children with CP.
The picture that came together was startling, specifically as I could now understand that the idea that CP as primarily a neurological disorder (i.e. one that only affected the brain and nerves) was incorrect. While the chain of events might start with the brain, there is much more to understand, in terms of secondary effects of the brain injury, before we can begin to engage with CP in a comprehensive and holistic way.
One example of collapsing structures due to metabolic dysregulation in Emma.
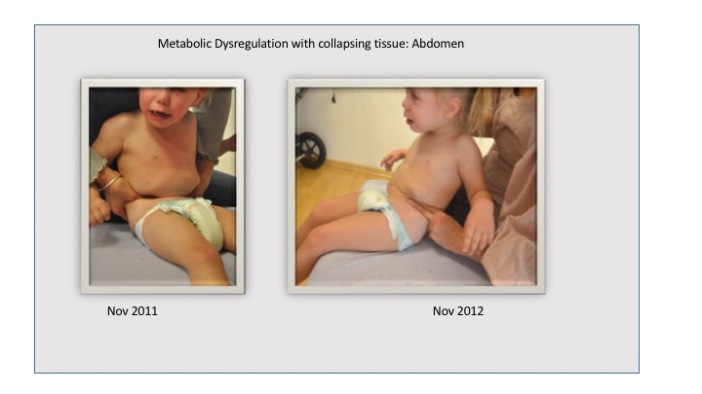
Note that in the first picture the examiner has to use her whole body to help Emma attain a sitting position. In the second, the abdominal collapse is markedly improved and she requires less support to attain the same sitting positioning. So as the collapse was addressed, the stability and strength improved. (Yay!)
Nutrition, my upcoming posts and the long-term investment
I have a great deal to share about how we helped Emma to learn to drink from a cup, to eat and how we optimised her nutrition and the results we have seen. I’d like to share this with you in detail, and in order to make it as helpful as possible for others as possible, I’m going to break this information up into a series of posts.
The key aspect of my nutritional approach with Emma is that I am focusing on her future. If nothing is done for metabolic dysregulation, it will get worse. Studies have found that kids with CP who become adults are prone to stop moving because they lose muscle strength. They lose function due to pain and deformity. They have an increased risk of insulin resistance, they may become obese (in the cases of milder CP) and their risk of heart attack is dramatically higher than healthy young adults of the same age.
Many of the nutritional approaches I have implemented for her will only bear fruit as she reaches adulthood. But, the science is clear, the short-terms gains of a high calorie diet (whatever she takes in, right?) is just not going to help her in the future if metabolic dysregulation isn’t addressed at the same time. Feeding her large handfuls of dietary supplements is also fraught with challenges and costs. Choosing the right tube food strategy has its own long list of challenges, too. Just like my approach to therapy choices, we need to be strategic and nimble to navigate these problems in our very sensitive and frail children.
I have had to really dig deep over the years to find beneficial foods of the right texture and composition that Emma will eat. Finding the right strategy to feed her and how to manage the intake of a child who does not “know” that she is thirsty and hungry is a further issue.
This is why I was so overjoyed at the beneficial effects of ABR. It is clear from the literature on connective tissue, and also from case studies, that ABR can change the metabolism of a child with CP in a powerful way. The changes we saw in Emma were not only structural, but also metabolic. Her body suddenly “knew” that it needed food and best of all, it suddenly “understood” how to metabolise the food we were giving. She has grown beautiful healthy muscle tissue over the past four years.
I am very excited to share the discoveries I have made in understanding my daughter’s condition, I am even more excited to say that I also understand what to do about it.
Learning through pain
There’s an isi-Zulu proverb from South Africa that I love:
“Utshani obulele buvuswa wumlilo.”
It translates as: the dry dead grass is made young and green by fire. Thus, often in life, one can only gain certain necessary positive results or learning after a drastic and even painful event.
This is why I write today.